Alternatives When Antihistamines Fail for Hives: 4 Solutions
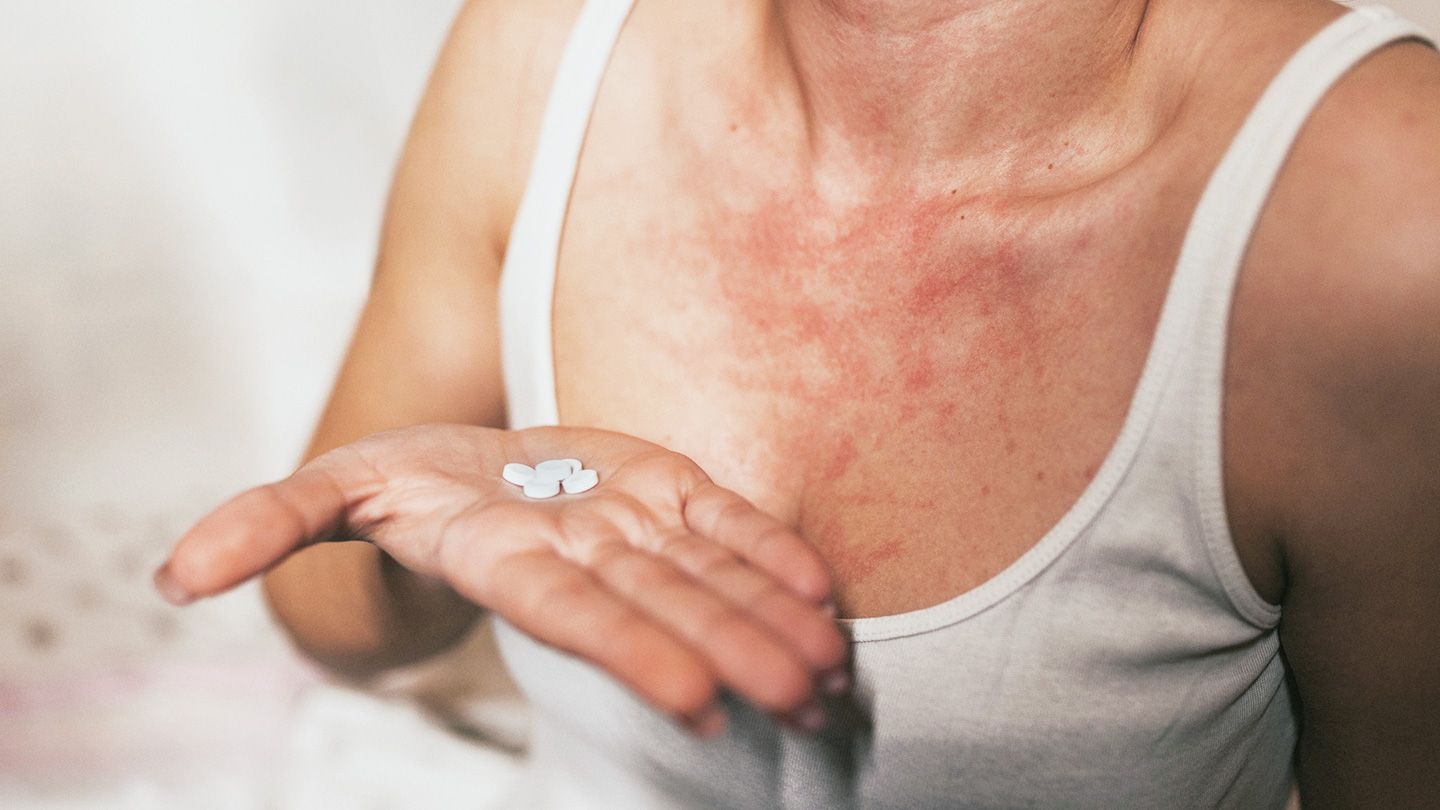
Hives are raised red welts or splotches that often cause itching, tenderness, and swelling. They can appear suddenly and occur anywhere on the body. For many individuals, over-the-counter antihistamines—also known as H1 antihistamines—are sufficient to provide relief from hives. These medications work by blocking histamine, a chemical released during inflammation, which may be triggered by allergens such as food or pollen, or by infections like viruses.
However, even if these medications initially help, they may become less effective over time. This is when other treatment options may need to be considered. According to Dr. Nicole Weiler, a dermatologist and clinical assistant professor at NYU Langone Health in New York City, the activity of hives can fluctuate, making antihistamines more or less effective at different times. When this happens, it's important to explore alternative treatments with a healthcare provider.
Here are four options your doctor might recommend if over-the-counter antihistamines stop working:
-
H2 Blockers
When OTC antihistamines like cetirizine (Zyrtec Allergy), fexofenadine (Allegra Hives), levocetirizine (Xyzal Allergy 24HR), and loratadine (Claritin) aren't effective, your doctor may suggest an H2 blocker. These medications, commonly used for gastrointestinal issues, target histamine receptors in the stomach and blood vessels, helping to reduce swelling and redness. Examples include cimetidine, famotidine, and nizatidine. Combining an H2 blocker with an OTC antihistamine can be very effective, according to Dr. Brendan Camp, a dermatologist in New York. If this approach doesn’t work, your doctor may move you off antihistamines altogether. -
Corticosteroids
If hives persist despite antihistamines, oral corticosteroids such as montelukast and prednisone may be prescribed. These medications reduce inflammation and mimic cortisol, a hormone naturally produced by the body. They can also help manage pain and suppress the immune system to prevent further histamine release. However, corticosteroids are not suitable for long-term use due to potential side effects such as mood changes, weight gain, and stomach irritation. -
Biologics
For frequent or severe hives that don’t respond to antihistamines or corticosteroids, biologic medications may be recommended. These drugs target specific components of the immune system, such as immunoglobulin E (IgE), which is involved in allergic reactions. One example is omalizumab (Xolair), which reduces IgE levels and helps alleviate symptoms. In April 2025, the FDA approved dupilumab (Dupixent) for chronic hives, targeting inflammatory proteins IL-4 and IL-13, which also play a role in IgE production. -
Lifestyle Changes
In addition to medical treatments, certain lifestyle adjustments can help manage hives. These include: - Identifying and avoiding food triggers with the help of a doctor
- Reducing exposure to airborne allergens like pet dander or pollen
- Using unscented detergents and soaps to avoid skin irritation
- Avoiding extreme temperature changes that may trigger or worsen hives
- Managing stress, which can exacerbate symptoms
- Wearing loose, lightweight clothing to prevent skin irritation
These changes can help reduce the frequency, duration, and severity of hives but are typically used alongside medication rather than as a substitute.
The Takeaway
Over-the-counter antihistamines are usually the first line of treatment for hives because they block histamine, a key factor in causing symptoms. If these don’t work, prescription antihistamines, corticosteroids, and biologics may be considered. Lifestyle modifications can also support treatment, but they are generally used in combination with medication. If hives become more frequent or severe and over-the-counter options aren’t effective, it’s important to consult a doctor for further evaluation and treatment options.
Post a Comment for "Alternatives When Antihistamines Fail for Hives: 4 Solutions"
Post a Comment